My Quick Lower Limb Clinical Neurological Examination
Following on from the Upper Limb Clinical Neurological Examination blog here are the details for my Lower Limb examination. Comments in regards to increasing neurological tone in regards to using the Jendrassick maneuver apply here also. See the Upper Limb neurological examination blog for further details.
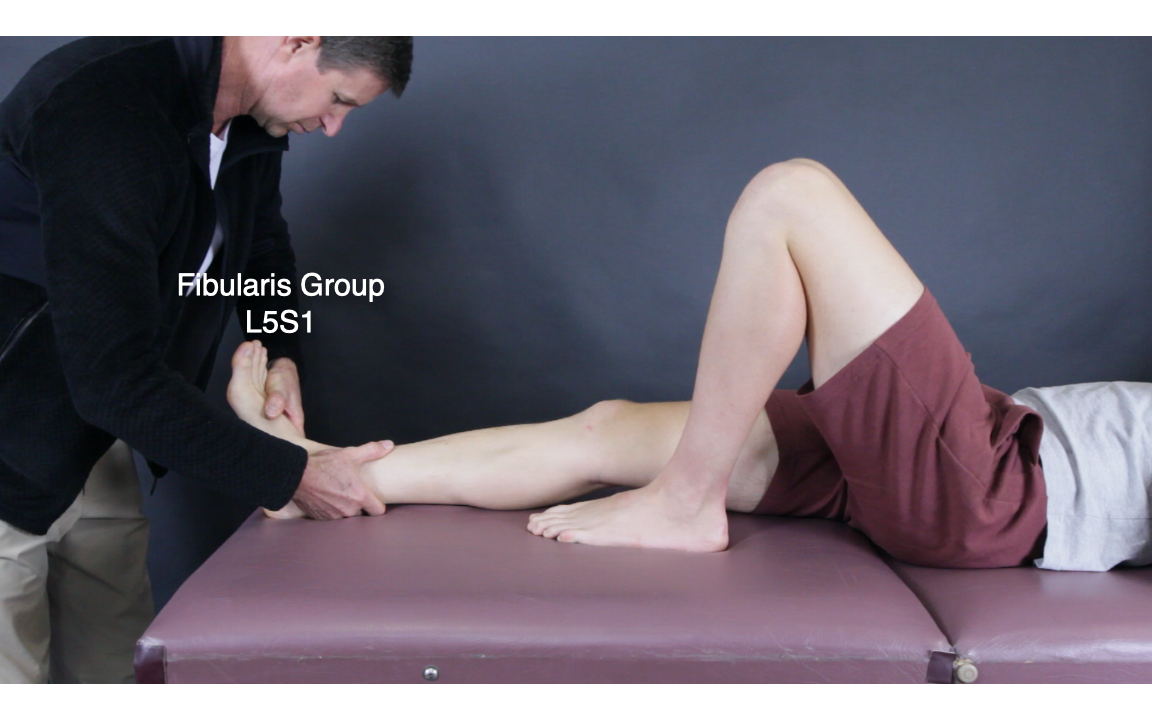
For power testing I use the following; Iliacus L2 (femoral nerve), Quadriceps L34 (femoral nerve), Tibialis Anterior L4 (deep fibular nerve | sciatic), Extensor Hallucis Longus L5 (deep fibular nerve | sciatic), Fibularis Longus/Brevis L5S1 (superficial fibular nerve | sciatic) and Triceps Surae S12 (Sciatic nerve). How weak is weak? For me it is not so much that the test is weak, more that the muscle test gives way - with no substance when challenged.
For reflex testing I use quadriceps L34, medial hamsstrings L5S1 and Triceps Surae S12. It is worth noting that if a trigger point is present in soleus it can limit/mask the spontaneous twitch of the triceps surae. Always compare to other side, as many people have reduced reflex response (more so with increased age) and we are not looking for generalities, rather specific variations. Also consider using alternative positions or the Jendrassik manoeuvre in situations of poor reflex testing. For increasing lower limb reflex responses, I normally use the a monkey grip, but apparently the teeth clench is more appropriate. In general in private practice you will be seeing clients with reduced or absent reflexes due to nerve compression, however be alert to the rarity that presents with hyper reflexia - indicating an upper motor neurone involvement.
In some ways sensation testing lacks the most clarity with regards to testing. Remember when testing sensation due to suspected nerve compression, you are initially testing for the reduction or absence of sensation. Clients often say an area feels numb, to which I ask, if I placed a lit cigarette on it would you feel it? Invariable the answer is 'yes I would feel it', so what they are describing is altered sensation rather than lack of sensation and this can have many causes. Vibration (placing a tuning fork on boney prominences) and pressure are conveyed by large myelinated fibers and these sensations are lost first when a nerve is compressed. I don't routinely test these clinically, rather I test light touch/pain/temperature using a monofilament as these sensations are lost after a period of compression. Monofilaments are traditionally used for testing diabetic related sensation loss, but are also a great way to have a calibrated applied pressure for skin sensation testing. Light touch is conveyed by the thinly myelinated (A delta) and un-myelinated nerve fibers (C fibers).
With regards to sensation, it is important to consider non-dermatonal sensation. Diabetic neuropathy needs to be considered if symptoms are bilateral, peripheral and nocturnal in nature. Also elements of chronic pain can be neuropathic, with non-dermatonal patterns, expanding receptive fields and sensitivity to cold testing.
In addition to nerve compression, I routinely give some consideration to nerve irritability (lower limb nerve provocation tests). Clients often present with dermatonal symptoms of pain and maybe parathesia, but no hard neurological signs. In these cases I am thinking chemical nerve irritation due to injury in the vicinity of a nerve root, but no direct compression. You can find out how I manage the common clinical presentation of acute low back pain here. Keep an eye out for older clients that have root level(s) chronically compressed (central or lateral stenosis). When non-irritated their slump test will be limited but not symptomatic (worth knowing for future reference). When they present with lumbar pain and you perform a slump test, it will be limited but this may be just a reflection of their underlying stenosis, rather than protective limited movement.
You can view a video of this clinical examination here.